AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
Back to Blog
Autologous induced pluripotent stem cells12/15/2023 One of the critical differences between iPSC and ESC is that iPSC can be induced from patients’ somatic cells. Organ transplantation is often the only curative therapy for end-stage organ failure however, low donor availability is currently a severe problem in some cases. This first challenge triggered the emergence of following iPSC-based clinical trials, and nearly 50 trials can be found as active status in ( ). The team led by Professor Masayo Takahashi of Riken Center for Developmental Biology in Japan successfully transplanted retinal pigment epithelial cells induced from patient autologous iPSC. In 2014, the first clinical trial was carried out with patients suffering from age-related macular degeneration. This fundamental feature of PSCs raised the possibility that PSCs, such as iPSCs and embryonic stem cells, can be an alternative source of transplant grafts. Under appropriate culture conditions, pluripotent stem cells (PSCs) can be directed their differentiation toward any cells or tissues. Their achievement opened the door for scientists to study organ or tissue regeneration, disease development, and drug discovery on the basis of iPSC-technology. Since Takahashi and Yamanaka have reported their breakthrough discovery, pluripotent stem cells became familiar not only to researchers but also to the public. The generation of induced pluripotent stem cells (iPSCs) boosted recent progress in the field of regenerative medicine. PSC-based technologies enable us to choose a new therapeutic option however, considering its safety from an immunological point of view should be of great importance for safe clinical translation of this technology. Also, our research group has recently proposed a concept that attempts to regulate recipient immune system by PSC-derived immunoregulatory cells, which results in prolonged survival of the same PSC-derived allografts. A couple of studies concerning such immunological issues have reported that genetic ablation of HLA molecules from PSC combined with gene transduction of several immunoregulatory molecules may be effective in avoiding immunological rejection. Even though pre-stocked and safety validated HLA-homozygous iPSCs are selected, immunological rejection may potentially occur because the causes of rejection are not always due to HLA mismatches.  
In order to minimize the risk of immune reaction, the banking of induced pluripotent stem cells (iPSCs) from donors with homozygous human leukocyte antigen (HLA) haplotype is planned in Japan. These findings support the feasibility of developing hiPSC-derived RPEs for treating macular degeneration.The development of pluripotent stem cell (PSC)-based technologies provides us a new therapeutic approach that generates grafts for transplantation. This differential immunogenicity is due in part to abnormal expression of immunogenic antigens in hiPSC-derived SMCs, but not in hiPSC-derived RPEs. In this context, autologous hiPSC-derived smooth muscle cells (SMCs) appear to be highly immunogenic, while autologous hiPSC-derived retinal pigment epithelial (RPE) cells are immune tolerated even in non-ocular locations. 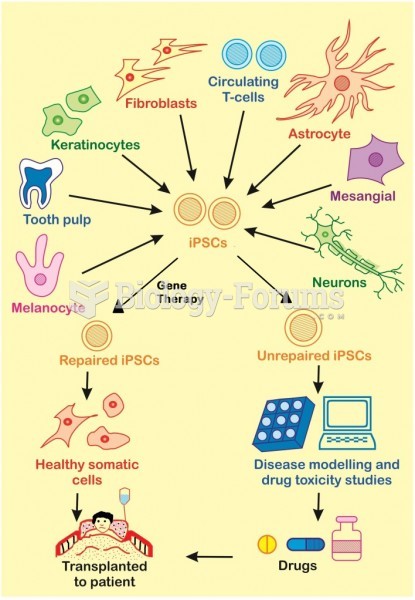
Using a humanized mouse model (denoted Hu-mice) reconstituted with a functional human immune system, we demonstrate that most teratomas formed by autologous integration-free hiPSCs exhibit local infiltration of antigen-specific T cells and associated tissue necrosis, indicating immune rejection of certain hiPSC-derived cells. However, the immunogenicity of autologous human iPSC (hiPSC)-derived cells is not well understood. The breakthrough of induced pluripotent stem cell (iPSC) technology has raised the possibility that patient-specific iPSCs may become a renewable source of autologous cells for cell therapy without the concern of immune rejection.
0 Comments
Read More
Leave a Reply. |
 RSS Feed
RSS Feed
